Overview
The type of vasectomy offered at Banyo Clinic is the “No Scalpel Vasectomy” (NSV). This procedure is less invasive than traditional vasectomies and does not require the use of any scalpels or knives. Instead, a specialized instrument is used to make a tiny opening in the skin – so small that no stitches are required for the healing process. The physician then locates the vas deferens via the tiny opening, then cuts and seals it to block the flow of sperm.
This type of minimally invasive surgery has less chance of complications and ensures a much shorter recovery time than other techniques.
Since its introduction in 1985, the No Scalpel Vasectomy has become a more popular option for couples around the globe – including approximately 30,000 men in Australia each year. It is less invasive than tubal litigation and is also less expensive with fewer chances of complications or extended recovery.
Vasectomy procedure information will be provided in depth and tailored to each individual, and your doctor will confirm that each patient is a suitable candidate prior to booking for the procedure.
Who will be performing my Vasectomy?

Dr Charles Elliott has been practising as a General Practitioner at Banyo Clinic since 2005. He completed his Bachelor of Medicine and Bachelor of Surgery at the University of Queensland in 1978, A Diploma of Child Health at the Royal College of Physicians of London in 1981, a Diploma of Obstetrics and Gynaecology at the Royal College of Obstetricians and Gynaecologists in 1982, and became a Fellow of the Royal Australian College of General Practitioners in 1987. In 2007, Dr Elliott completed his Certificate of Australian Skin Cancer Medicine at the Skin Cancer Society of Australia, and in 2013 completed his Masters of Medicine at the University of Queensland. Dr Elliott first started doing vasectomies in the 1980’s after learning his technique from well-known Brisbane vasectomist Dr Bruce Errey. In 2019, Dr Elliott wanted to refine his technique, and so completed his certified vasectomy training under the watchful eye of Dr Doug Stein at the Doug Stein and John Curington Vasectomy and Reversal Clinic in Lutz, Florida.
What should I do before my vasectomy?
- Ensure you have had a consultation with Dr Charles Elliott and have been approved for the procedure.
- Understand the alternatives to vasectomy and ensure that you are confident in your choice.
- Shave the front of your scrotum the day before the procedure – an alcohol solution is used to clean the area, and this may sting soon after a shave. Use no powder or deodorant on or around the scrotal area on the day of the procedure.
- Organise to have somebody drive you home from the procedure and ensure you have allowed a sufficient time to rest and recline afterwards.
- Do not take any aspirin medication for five days prior.
- Make sure you eat before your procedure – nervous hungry men are more likely to become lightheaded during or post their vasectomy.
- Sign the vasectomy procedure consent form.
What happens during the vasectomy?
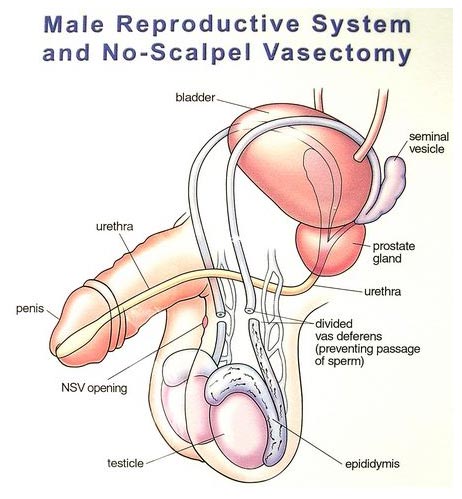
Photo © 1994, 1997, 2001 Advanced Meditech International, Inc. By permission from Dr Doug Stein, July 2019.
First, anaesthetic is applied using a spray applicator to numb the vas tubes and the scrotal skin, and a short time passes while the anaesthetic is absorbed and begins to work in numbing the area.
Next, access to the vas deferens is gained by using a special instrument that creates a single opening on the front side of the scrotum approximately ¼” long. The vas deferens sit just beneath the scrotal skin and so are very easy to reach. As the cut is so small, it usually only takes a couple of hours to heal and requires no stitches. And because the blood vessels in the skin are spread apart rather than cut, the bleeding is far less than if a scalpel were to be used.
Blocking the vas tubes is completed by using fine surgical scissors to divide the left and right tubes individually at approximately one inch above each testicle. One severed tube end is cauterized and then separated from the other end by a layer of tissue to ensure the ends can never again communicate.
Finally, a simple dressing is applied, and a scrotal support or jockstrap will be supplied if you don’t have one which is to be worn overnight, and reapplied the following day.
Dr Elliott will phone you the day after the vasectomy to check in in case you have any concerns.
FAQs
Does a vasectomy procedure hurt?
No. Local anesthetic is used which can feel uncomfortable, but once it has taken effect there should be no pain during the procedure. Some men report feeling a slight tugging sensation as the GP manipulates the vasa. Pain, if any, is usually only present during the recovery.
How long will it take to recover?
Usually 2 – 7 days. Directly after the procedure, it is recommended that the patient spend a relaxed evening reclining or lying down and using paracetamol or ibuprofen for pain relief – there should be no need for any ice packs. Having daily showers the morning after the procedure are also recommended. Returning to work depends on the type of work, for example, those with office jobs can return to work the next day – walking and driving is fine. Anything more strenuous such as heavy lifting, yardwork, or physical exertion and sports should be avoided for 2 days post-procedure. Scrotal support or tight underwear should be worn for the 2 days post procedure, and during any physical activities for 7 days post-procedure.
How long until I can have sex again?
As soon as two to seven days after the procedure, you should be able to begin having sex. Each person is different, and it is always best to wait until pain is gone and tenderness is minimal, though rule of thumb is always no ejaculations for at least 2 days. It is normal for some blood to appear in the semen for the first few ejaculations, and possibly even months after the procedure. You will need to use your usual contraceptive methods as you can still get your partner pregnant until you have returned a negative sperm result.
How will my performance be affected?
All hormonal and sexual functions remain completely unchanged, as does the penis and testes. The only interruption is at the tubes which prohibits sperm from the testes to be added to the semen. Ejaculations, erections, hair, voice and body all remain unaltered, as does your interest in sex. Vasectomy is not a castration, it just means that your semen will no longer contain any sperm, and the and the body will continue to absorb unused sperm as it always has.
When can I stop using contraception?
After the vasectomy and at least 12 weeks and 20 ejaculations have passed, you will need to supply a semen sample to your local Pathology Laboratory, as directed by your GP. Your vasectomy should not be considered complete until the GP has notified that you have successfully returned a negative sperm result.
What are some normal complications?
The No Scalpel Vasectomy technique is a very low risk procedure. However, as with all procedures and forms of contraception, some complications are possible.
It is normal to experience some discoloration around the vasectomy site, usually four days after the procedure. This is just blood from the vasectomy site which surfaces to the skin and creates a purple-blue mark.
Approximately one in twenty men may develop swelling and discomfort on one or both sides of the scrotum post-procedure. This is usually a normal inflammatory response for sperm absorption and recycling, but if exaggerated can become tender for the patient. This can happen any time between three days to three months post-procedure and can be easily managed with a three to five-day course of ibuprofen, 600mg three times a day. Once the tenderness has receded, continue to take the ibuprofen for one more day, though do not take for more than seven days.
Haematoma and/or infection: Haematomas and infections are one of the most common complications from a vasectomy procedure, though are still considered very rare – due to the small size of the opening made in the scrotum, the chances of blood vessels causing bleeding is reduced, as are infections.
Granuloma: Sperm granuloma is a hard and occasionally painful lump that may form because of the cut to the vas deferens. It is usually the size of a pea and resolves by itself over time with the help of mild pain relievers and using scrotal support.
Congestion: Congestion is the term given to pressure caused by sperm in the lower vas deferens, testes and epididymis any time between two and twelve-weeks post procedure, and usually resolves itself over time.
Failure: Vasectomy is not a 100% guarantee of success. Even after the procedure, it can be possible in very rare cases for sperm to find its way across the void left between the two blocked ends of the vas deferens. In these very rare instances – referred to as recanalization – failure can be detected by completing the sperm count at twelve weeks post-procedure. However, in even more extreme cases, recanalization has occurred up to years later.
In any case, if you have any concerns, pain or abnormal symptoms post procedure, it is best to visit your GP or return to Dr Charles Elliott for review and clinical advice.
Are there long-term risks?
No. There is no evidence to suggest that men who have had vasectomies are at any higher risk of cancer, heart disease or other health problems than men who have not had a vasectomy.
Can I reverse my vasectomy?
Reversal is possible, but not guaranteed. While reversal procedures do exist, they are expensive and do not guarantee that fertility can be restored. The chance of successful reversal decreases each year following the vasectomy, so it should be considered a permanent procedure.
How do I book?
By phoning Banyo Clinic reception on 32675088 – ensure you have booked a consultation appointment with Dr Charles Elliott.
After your initial consultation, Dr Elliott will advise if the No Scalpel Vasectomy procedure can then be scheduled, and we will book this for you after your appointment.
Where can I find more information?
Feel free to head over to Dr Doug Stein’s Vasectomy website for more detailed information about the No Scalpel Vasectomy technique practiced at Banyo Clinic.

